Tau and pTau Biomarkers in Alzheimer’s Disease
A Comprehensive Guide to Tau Protein, Phosphorylated Tau, and Their Role in Diagnosis and Research
Published March 2026 | Neurology & Biomarker Research | Estimated reading time: 10 minutes
Alzheimer’s disease (AD) affects more than 55 million people worldwide and remains one of the most complex and devastating neurodegenerative conditions known to medicine. Among the most important advances in understanding — and ultimately diagnosing — Alzheimer’s disease has been the identification of specific biological markers, or biomarkers, that signal the presence and progression of the disease. Two of the most clinically significant of these aretau (τ) protein and phosphorylated tau (pTau). This article explores what tau and pTau biomarkers are, how they are measured, what they tell us about Alzheimer’s pathology, and why they are central to the future of diagnosis and treatment.
What Is Tau Protein?
Tau is a microtubule-associated protein that plays a critical role in maintaining the structural integrity of neurons. Under healthy conditions, tau binds to and stabilizes microtubules — the internal scaffolding that gives neurons their shape and supports the transport of nutrients and cellular cargo. Tau is encoded by the MAPT gene (Microtubule-Associated Protein Tau) on chromosome 17 and is expressed primarily in neurons of the central nervous system.
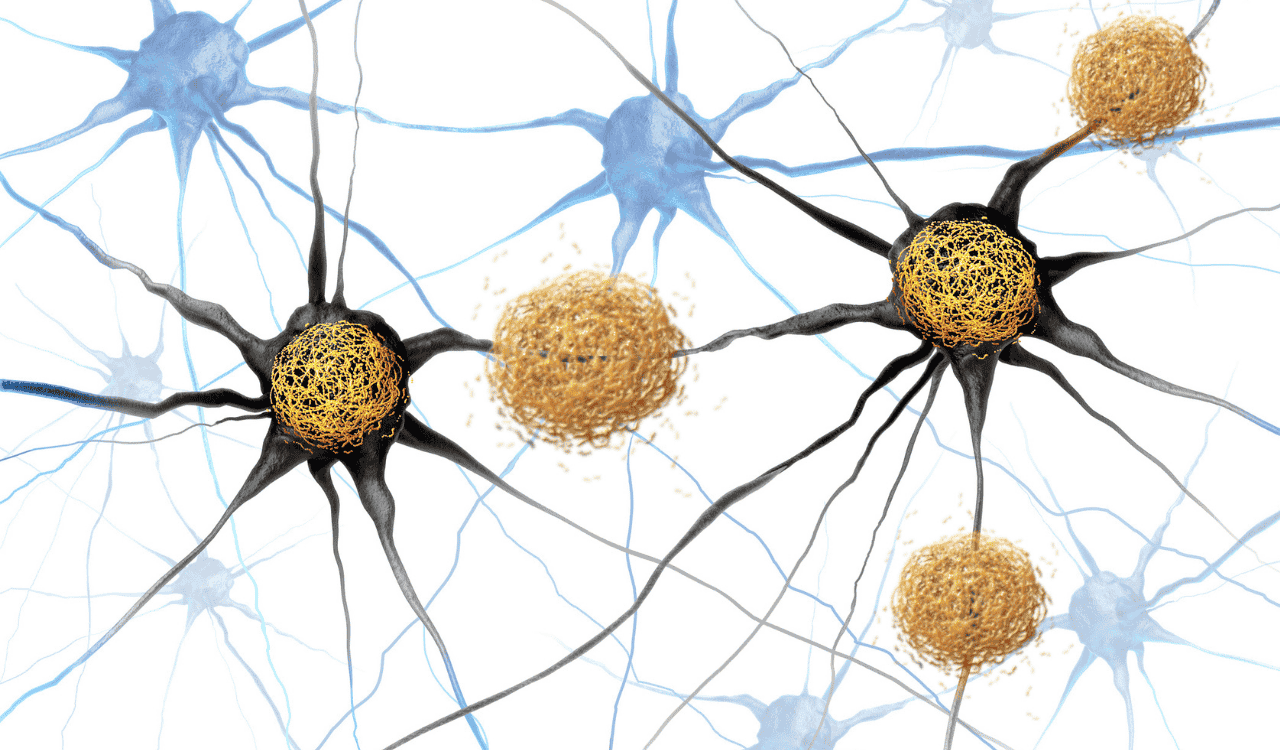
In a healthy brain, tau is appropriately phosphorylated — meaning phosphate groups are added to certain amino acid sites — as part of normal regulatory processes. However, in Alzheimer’s disease and other tauopathies, tau becomes hyperphosphorylated: phosphate groups accumulate excessively at abnormal sites. This hyperphosphorylated tau loses its ability to bind microtubules and instead aggregates into paired helical filaments (PHFs), which coalesce into the neurofibrillary tangles (NFTs) that are one of the hallmark pathological features of Alzheimer’s disease.
Tau in Alzheimer’s Pathology: Neurofibrillary Tangles
The formation of neurofibrillary tangles is directly linked to neuronal death and cognitive decline. As tau detaches from microtubules and misfolds, neurons lose their structural support and transport capacity, leading to synaptic dysfunction and eventual cell death. The spread of tau pathology across the brain follows a predictable anatomical pattern first described by Heiko and Eva Braak — known as Braak staging — progressing from the entorhinal cortex to the hippocampus and ultimately throughout the neocortex.
This staging system has proven invaluable both for post-mortem diagnosis and, increasingly, as a framework for interpreting biomarker data in living patients. Understanding how and where tau spreads informs which biomarker measurements are most informative at different disease stages.
Key Tau Biomarkers: Total Tau and Phosphorylated Tau
Total Tau (t-Tau)
Total tau (t-tau) refers to all forms of tau protein detected in cerebrospinal fluid (CSF) or blood plasma, regardless of phosphorylation state. Elevated t-tau in CSF reflects neuronal damage and death — it rises as neurons are injured, releasing their intracellular tau into surrounding fluid. Elevated t-tau is not specific to Alzheimer’s disease; it can be elevated following traumatic brain injury, stroke, or other neurodegenerative conditions. Nonetheless, it remains an important component of the AD biomarker profile.
Phosphorylated Tau (pTau)
Phosphorylated tau (pTau) is more disease-specific than total tau. Different phosphorylation sites on the tau protein are measured using site-specific assays, and several have proven diagnostically and prognostically important:
- pTau-181 (threonine 181): The most widely used pTau biomarker, pTau-181 is elevated in Alzheimer’s disease and has been validated in both CSF and plasma. It correlates with amyloid burden and helps differentiate AD from other dementias.
- pTau-217 (threonine 217): Emerging evidence suggests pTau-217 may be the most sensitive and specific marker for Alzheimer’s pathology, rising earlier in the disease course and tracking more closely with amyloid PET imaging results.
- pTau-231 (threonine 231): pTau-231 increases very early in AD, possibly before amyloid PET becomes positive, making it a promising marker for the preclinical detection of Alzheimer’s pathology.
How Are Tau Biomarkers Measured?
Cerebrospinal Fluid (CSF) Analysis
Historically, tau biomarkers have been measured in cerebrospinal fluid (CSF) obtained via lumbar puncture. CSF is in direct contact with the brain and therefore provides a rich source of neurochemical information. The classic AD biomarker profile in CSF includes low amyloid beta-42 (Aβ42), elevated t-tau, and elevated pTau-181 — often described as the “ATN” framework (Amyloid, Tau, Neurodegeneration). CSF analysis remains the gold standard for tau biomarker measurement, with high sensitivity and specificity.
Blood-Based Plasma Biomarkers
One of the most transformative developments in Alzheimer’s biomarker research has been the advent of ultrasensitive plasma assays capable of detecting minute quantities of tau in blood. This is technically challenging because plasma tau concentrations are roughly 100-fold lower than in CSF, and the blood-brain barrier limits the amount of brain-derived protein that enters the bloodstream.
Advances such as the Single Molecule Array (Simoa) platform and mass spectrometry-based approaches have made plasma pTau-181, pTau-217, and pTau-231 measurable with clinically relevant accuracy. Several large studies have demonstrated that plasma pTau-217, in particular, can differentiate AD from other neurodegenerative diseases with an accuracy comparable to CSF or amyloid PET imaging — a major step toward accessible, scalable screening.
PET Imaging
Tau positron emission tomography (PET) imaging uses radioactive tracers — such as flortaucipir (AV-1451), MK-6240, and PI-2620 — that bind to tau aggregates in the living brain. Tau PET provides a spatial map of tau deposition, enabling visualization of Braak staging in vivo. While highly informative, tau PET is expensive, not universally available, and involves radiation exposure, limiting its use to research settings and specialized clinical contexts.
Clinical Utility: Diagnosis and Differential Diagnosis
The combination of amyloid and tau biomarkers is central to the 2018 NIA-AA Research Framework for defining Alzheimer’s disease biologically rather than clinically. Under this framework, an individual is considered to have AD pathology when both amyloid (A) and tau (T) biomarkers are positive, regardless of symptoms.
Tau biomarkers — especially pTau species — are also valuable for differential diagnosis. Because different neurodegenerative diseases have distinct tau pathologies (e.g., 3R tau in Pick’s disease vs. 4R tau in corticobasal degeneration and progressive supranuclear palsy), pTau profiles can help clinicians distinguish between conditions that may present similarly.
In 2024 and 2025, regulatory agencies in Europe and the United States began reviewing data supporting the use of plasma pTau-217 as a diagnostic aid for Alzheimer’s disease, signaling a shift toward blood-based biomarkers entering mainstream clinical practice.
Tau Biomarkers as Prognostic Tools
Beyond diagnosis, tau biomarkers carry significant prognostic value. Higher levels of CSF or plasma pTau correlate with faster cognitive decline, greater hippocampal atrophy, and worse clinical outcomes. Longitudinal studies have shown that rising pTau levels precede clinical symptoms by years to decades, making these markers particularly valuable for identifying individuals in the preclinical phase of Alzheimer’s disease — before irreversible neuronal loss has occurred.
This prognostic capacity is directly relevant to clinical trials: tau biomarkers are increasingly used as enrollment criteria and outcome measures in trials of disease-modifying therapies, helping to ensure that participants have confirmed AD pathology and that treatment effects can be monitored objectively.
Tau Biomarkers and Therapeutic Development
The tau protein is not only a diagnostic target but also a therapeutic target. Several strategies are under active investigation:
- Anti-tau immunotherapy: Monoclonal antibodies targeting tau aggregates or phosphorylated tau epitopes aim to reduce tau burden. Semorinemab, gosuranemab, and tilavonemab have been tested in clinical trials, with mixed results highlighting the complexity of targeting tau in established disease.
- Tau aggregation inhibitors: Small molecules such as hydromethylthionine (LMTX) seek to prevent tau from forming toxic aggregates. Clinical results have been inconclusive, though research continues.
- PROTAC and ASO approaches: Proteolysis-targeting chimeras (PROTACs) and antisense oligonucleotides (ASOs) targeting MAPT expression aim to reduce tau production at the source. BIIB080, an ASO targeting MAPT, showed significant reductions in CSF tau in a Phase 1/2 trial reported in 2023.
Tau biomarkers serve as pharmacodynamic readouts in these trials — allowing researchers to confirm target engagement and dose optimization before committing to large efficacy studies.
Challenges and Future Directions
Despite remarkable progress, several challenges remain in the tau biomarker field:
- Standardization: Assay variability across laboratories and platforms complicates cross-study comparisons. International harmonization efforts, including the Global Biomarker Standardization Consortium (GBSC), are working to address this.
- Specificity: While pTau-217 shows excellent specificity for AD, elevations can also occur in other amyloid-positive conditions. Combining tau with amyloid and neurodegeneration markers improves overall diagnostic accuracy.
- Pre-analytical factors: Blood-based biomarkers are sensitive to sample handling, storage conditions, and comorbidities such as kidney disease, which can affect plasma tau levels independently of brain pathology.
- Ethnic and genetic variability: Reference ranges and cutoff values may vary across populations and with genetic factors such as APOE4 status. Inclusive, diverse cohort studies are needed to establish universally applicable reference standards.
Looking ahead, the field is moving rapidly toward multi-analyte panels that combine tau species with amyloid markers (e.g., Aβ42/40 ratio), neurodegeneration markers (e.g., neurofilament light chain, NfL), and synaptic biomarkers (e.g., neurogranin, SNAP-25) for comprehensive, blood-based AD staging. Artificial intelligence and machine learning are being applied to integrate these complex datasets into clinically actionable risk scores.
Conclusion
Tau and pTau biomarkers have fundamentally transformed our understanding of Alzheimer’s disease — from a clinical syndrome diagnosed after significant neuronal loss to a biological process detectable years or even decades before symptoms emerge. The evolution from CSF-only measurement to validated plasma assays represents one of the most significant advances in dementia research in decades, promising a future where Alzheimer’s can be diagnosed with a routine blood test.
As therapeutic trials advance and regulatory landscapes evolve, tau biomarkers will be indispensable tools — for earlier diagnosis, better patient selection, objective monitoring of treatment effects, and ultimately, for realizing the goal of disease modification in Alzheimer’s disease. Continued investment in biomarker research, standardization, and equitable access to testing will be essential to translate these scientific achievements into broad clinical benefit.
References and Further Reading
- Jack CR Jr. et al. (2018). NIA-AA Research Framework: Toward a biological definition of Alzheimer’s disease. Alzheimer’s & Dementia, 14(4), 535–562
- Janelidze S. et al. (2020). Plasma P-tau181 in Alzheimer’s disease: relationship to other biomarkers, differential diagnosis, autopsy findings, and longitudinal progression to Alzheimer’s dementia. Nature Medicine, 26, 379–386
- Barthélemy NR et al. (2020). Cerebrospinal fluid phospho-tau T217 outperforms T181 as a biomarker for the differential diagnosis of Alzheimer’s disease and PET amyloid-positive patient identification. Alzheimer’s Research & Therapy, 12, 26
- Blennow K., Zetterberg H. (2021). Biomarkers for Alzheimer’s disease: current status and prospects for the future. Journal of Internal Medicine, 284(6), 643–663
- Gauthier S. et al. (2023). World Alzheimer Report 2023: Reducing dementia risk. Alzheimer’s Disease International
- Teng E., et al. (2022). Safety, tolerability, and pharmacodynamics of BIIB080, an antisense oligonucleotide targeting tau. JAMA Neurology, 79(6), 594–604
- Braak H., Braak E. (1991). Neuropathological stageing of Alzheimer-related changes. Acta Neuropathologica, 82(4), 239–259
- Alzheimer’s Association. (2024). Alzheimer’s disease facts and figures. Alzheimer’s & Dementia, 20(5), 3708–3821



Leave a Reply